Peripheral Vascular Disease (PVD) is a peripheral circulation disorder that affect blood vessels outside the heart and brain. PVD that develops only in the arteries is called Peripheral Arterial Disease (PAD). PAD develops most commonly as a result of atherosclerosis, or hardening of the arteries, which occurs when cholesterol and scar tissue build up, forming a substance called plaque inside the arteries.
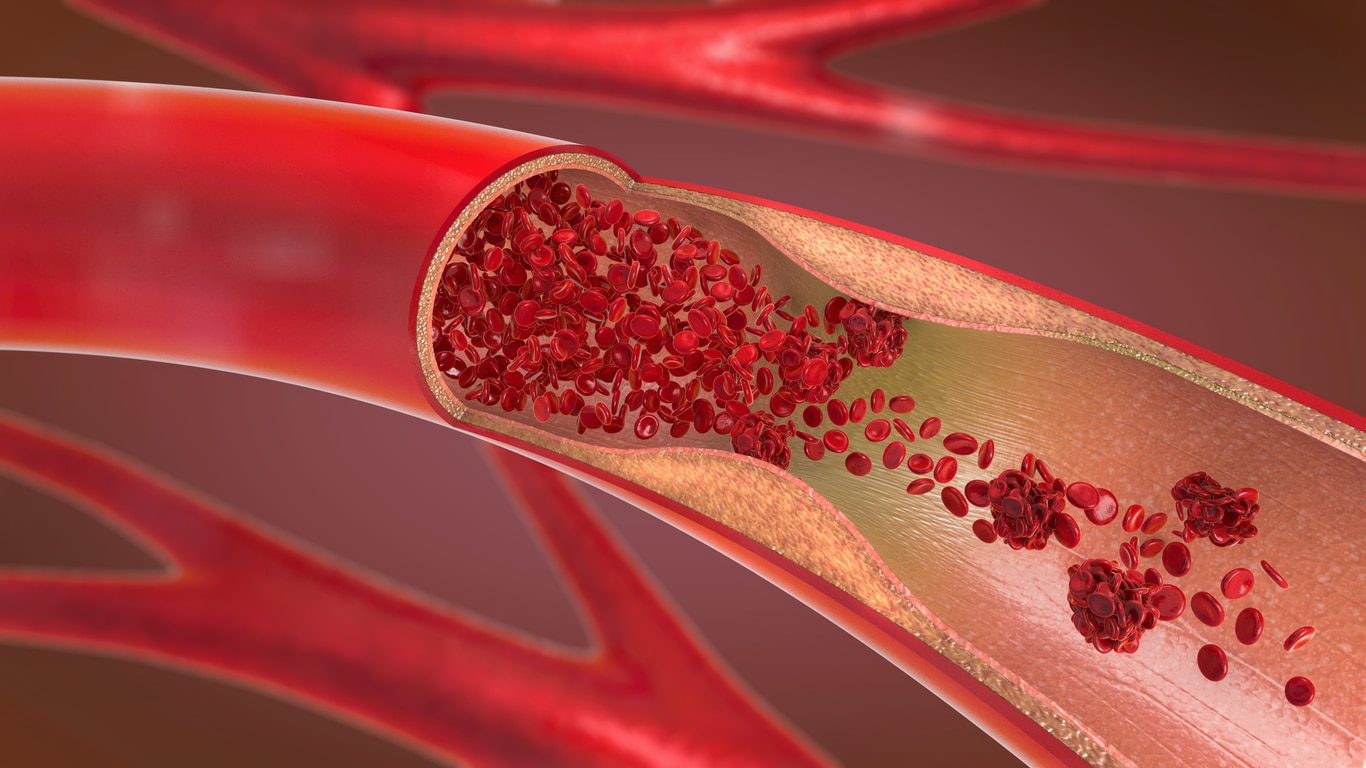
This is a very serious condition. The clogged arteries cause decreased blood flow to the arms, or more commonly, the legs. This can result in pain when walking and eventually gangrene and/or amputation.
*Rights reserved with the owner of the video.
Signs and Symptoms of PAD & PVD:
The most common symptom of PAD and arterial insufficiency is called intermittent claudication, which is painful cramping in the leg or hip that occurs when walking or exercising and typically disappears when the person stops the activity. Other symptoms include: numbness, tingling and weakness in the lower legs and feet, burning or aching pain in feet or toes when resting, sore or wound on the leg or foot that won’t heal or is slow to heal, cold legs or feet, color changes in skin of legs or feet, hair loss on legs, pain in the legs or feet that wakes you up at night or pain at rest. All of these symptoms can be indicative of poor circulation in lower extremity arteries.
PVD that develops in the deep veins in the body is usually caused from claudication and is called Deep Vein Thrombosis (DVT).
How does Peripheral artery disease affect daily life?
Peripheral artery disease can be a chronic or recurring condition that creates difficulty performing daily activities. Studies indicate that women tend to develop more severe symptoms than men, and that the severity of their symptoms could impair quality of life to the point of depression. The ways in which PAD may affect daily life include the following:
- Leg or foot pain. The insufficient circulation of blood to the legs can cause pain that ranges from a dull throbbing to severe aching. Pain may prevent the patient from getting a good night's sleep and from walking comfortably.
- Slow wound healing. The body relies on oxygenation from the blood to repair itself. With PAD, blood is not flowing sufficiently to the legs and feet so these areas are particularly vulnerable to scarring and slow healing if bumped, scraped, or cut. Infection is the primary concern related to slow-healing wounds
- Heaviness and fatigue in the legs. Blood circulation in the legs is not only necessary for healing but also for energy levels and healthy movement. Claudification, the sensation of heaviness or fatigue in the leg muscles, can make it difficult to ride a bike, climb stairs, or walk.
The causes of Peripheral Artery Disease
Peripheral artery disease is caused by a blockage in the arteries of the leg or arm. Our arteries are like hollow tubes through which blood flows. These tubes are smooth and stretchy. As a result of predisposed risk factors and lifestyle choices, fatty deposits can attach themselves to the inside walls of blood vessels. Once fatty deposits start to stick, they build up. The body attempts to heal itself from the fatty buildup by making the vessel walls sticky. This healing response allows other substances in the bloodstream, including calcium, proteins, and inflammatory cells, to become stuck. Together with the fatty deposits, this debris forms a plaque that narrows the artery.
The areas of the body PAD & PVD effects
Peripheral arterial disease is atherosclerosis that develops in the arteries of the legs or, less commonly, the arms.
Patient Testimonial
"Friendly, courteous, professional. This is the absolute best medical staff in the Fredericksburg area for this medical specialty. Anyone with a vascular condition please do yourself a favor and call them."
How is PVD diagnosed?
In order to diagnose PVD, the physician will begin by taking a complete medical history and physical exam. Several tests may be used to diagnose PVD. They are:
- Measuring the pulses in your legs and feet
- Doppler ultrasound
- Ankle-Brachial Index (ABI)
- Pulse Volume Recording (PVR)
- Angiography
Arterial Duplex Ultrasound Scan
An Arterial Duplex Ultrasound is a non-invasive imaging scan that uses sound waves to create a color map of the arteries in your leg(s) to identify narrowing of your vessels that may be causing leg pain when walking or at rest, ulcers of the foot, ankle, heel or toe(s), or skin discoloration.
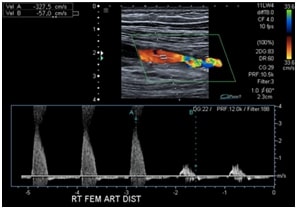
Peripheral Angiograms:
Abdominal aortograms with runoff are arteriograms of the lower abdominal aorta and arteries in the legs. This exam is often done when the patient has pain in the calf muscle after walking a short distance, discoloration of the toes or feet, non-healing wounds or ulcers, or a “cold” foot.
Treatment Options we offer:
Once angiographic images have been obtained and problem areas identified, some of the methods we utilize to treat those diseased areas are Angioplasty, Thrombectomy, Atherectomy, or Stent placement.
Angioplasty uses a balloon catheter to open up a stenotic area (or area of narrowing) in a blood vessel.
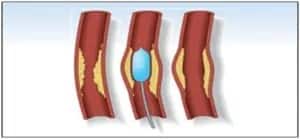
Thrombectomy is a process in which thrombus (or clot) is mechanically removed from the body using specialized equipment.
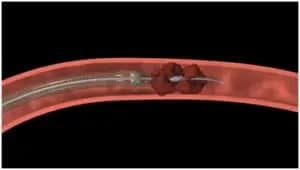
Atherectomy refers to the mechanical removal of atheroma or atherosclerosis from the inside of the vessels in the body, using specialized catheters and equipment.
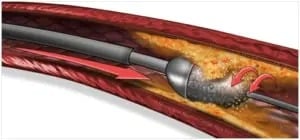
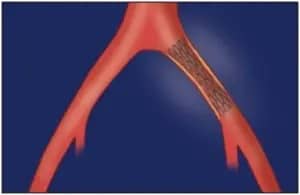
Stents are small metal scaffolds that can be placed in order to maximize the inner diameter of vessels and help to keep it open.
Is there anything I can do for PAD on my own?
To control PAD, you should stop smoking and walk every day. It is also beneficial to limit the consumption of high-fat and high-sugar foods and to talk with your primary care physician about the management of risk factors such as diabetes, high cholesterol and high blood pressure.
Recovery from PAD treatments
There may be some recovery time needed after certain PAD treatments. For example, patients who undergo angioplasty to open clogged arteries may have various activity restrictions that last a few weeks. Most interventional procedures are performed on an outpatient basis. Before the day of treatment, patients receive detailed pre-and post-procedure instructions to help in their recovery. Our team is available to answer questions that may arise.

What are the Risk Factors for Peripheral Artery Disease?
Some of the risk factors that contribute to the development of peripheral artery disease are beyond your control. These include:
- Advanced age (over age 65)
- Having risk factors for atherosclerosis at any age
- Having Type 2 diabetes and one or more additional risks for atherosclerosis
- Family history of stroke or cardiovascular disease
While you cannot control genetic and age-related factors that put you at risk of peripheral artery disease, you can control one or more of the lifestyle factors for this condition. These include:
- Manage your risk for Type 2 diabetes
- Do not smoke
- Keep your blood pressure under control through screenings and healthy diet and exercise habits
- Maintain healthy cholesterol levels through diet and exercise
- Engage in a supervised exercise program if that is advised by your doctor
What are the Benefits of Angioplasty or Stenting for Peripheral Artery Disease?
When possible, doctors attempt to address peripheral artery disease with the most conservative treatments, including prescription medications and lifestyle changes. If your symptoms are severe or your diagnostic testing reveals significant arterial blockage, your doctor may advise you to have angioplasty or stenting. These procedures are advantageous because they are much more conservative than bypass surgery and carry fewer risks. There is no need to receive general anesthesia for angioplasty or stenting, and you don't need to stay overnight in the hospital. In fact, neither of these procedures even involves significant incisions, only a small nick in the skin through which the doctor inserts a thin, flexible tube. Because angioplasty and stenting are such minimally-invasive procedures, you can expect to resume normal activities sooner than you would if you received surgical treatment to unblock clogged arteries.
Are Angioplasty and Stenting Permanent Solutions for Peripheral Artery Disease?
Angioplasty and stenting are two separate procedures that are considered when necessary to address the symptoms of peripheral artery disease. The objective of each of these non-surgical treatments is to unblock the obstructed arteries and restore good circulation to the affected limb. While these procedures can unblock the obstruction that is present, neither reverses the underlying conditions that have led to the development of the blockage. The results of your procedure may be long-lasting. The treated artery may never require re-treatment. However, your atherosclerosis may continue if you do not make the changes that are necessary to resolve the factors that are contributing to it.
After having an angioplasty or stent placement, you'll need to follow your doctor's recommendations for cardiovascular health management. If you're prescribed medication, take it as directed. If you smoke, quit. If your diet is one that contributes to diabetes, high blood pressure, high cholesterol, and other unhealthy conditions, seek the help that you need to develop better dietary habits. Every step that you take toward better glucose management and cardiovascular health is worth it.
Schedule Your Consultation Today!
Interested in learning more about Peripheral Arterial Disease Treatment with Vascular Institute of Virginia? Call 703-763-5224 to schedule your consultation today! Our practice serves Fredericksburg, Woodbridge, Fairfax & all nearby areas in Virginia.